Treatment of children with sleep-disordered breathing
From Martin Bailey FRCS
Sleep-disordered breathing affects approximately 12% of children, and consists of an abnormal breathing pattern during sleep which may include snoring, mouth breathing, and pauses in breathing. It is most commonly caused by large tonsils and adenoids.
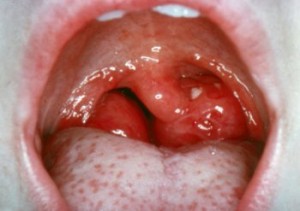
Very large, obstructive tonsils meeting in the midline
In mild cases it characteristically consists of snoring and a disturbed sleep pattern at night, with mouth-breathing and sometimes hyperactivity during the day.
In severe cases the child may struggle to breathe while asleep, and even momentarily stop breathing (‘obstructive sleep apnoea’). Such severe obstruction is potentially serious because it puts a strain on the heart and the lungs, and may affect growth and development. Even one obstructive episode per hour is significant in children, and the resulting sleep fragmentation can over time result in intellectual impairment with a reduced IQ1.
Treatment is removal of the tonsils and adenoids, and usually this is dramatically curative. However, an Australian review2 has indicated that in Australia and New Zealand only 1 in 7 of children who would benefit from this surgery are actually being treated, and the figures may well be worse for children missing out on treatment in the UK.
1. Behavior, cognition, and quality of life after adenotonsillectomy for paediatric sleep-disordered breathing: summary of the literature; Garetz SL; Otolaryngol Head Neck Surg 138(1): S19-S26 (January 2008)
2. A joint Position Paper of the Paediatrics and Child Health Division of the Royal Australasian College of Physicians and the Australian Society of Otolaryngology, Head and Neck Surgery, 2008 Sydney
